Team:UCSF/Project
From 2010.igem.org
|
Project DescriptionThe UCSF 2010 iGEM team aims to combat one of the leading causes of death worldwide - cancer. Globally, cancer accounts for nearly 1 of every 8 deaths. The number is projected to rise continuously as 1,530,000 new cancer cases are expected to be diagnosed just this year alone. We attempt to fight cancer by enhancing the immune system’s functions using synthetic biology. Specifically, our goal is to turn natural immune cells into Synthetic Killers that can:
First, let me tell you a little about the immune system natural response against cancer.
Introduction to Killer Immune CellsIn the mammalian immune system, many types of while blood cells with specific functions and responsibilities constantly work to defend the body against disease. There are two types of immune cells that are at the center of the fight against cancer: natural killer (NK) cells and cytotoxic T cells. NK cells are part of the innate immune response and survey the body for any unusual activity before signaling for additional help. If necessary, the activation of NK cells will then signal for a secondary response in which cytotoxic T cells are called to assist in the removal of the remaining unhealthy/cancerous cells. In this project, we will be referring to these cells as Killer Immune Cells. Both of these types of killer cells go through a similar process from detection to elimination of the cancer cell.
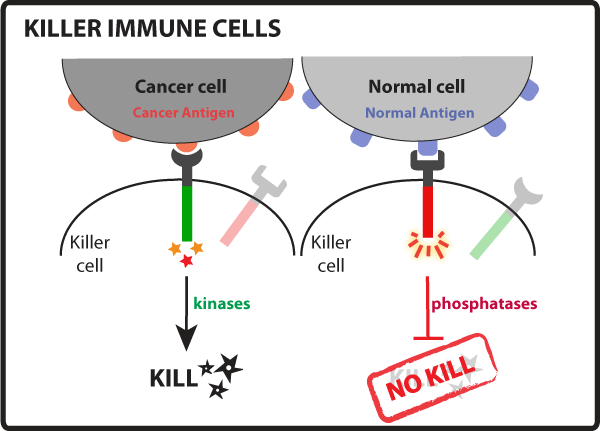
1 - Detection of Cancer Cells by Killer Immune Cells Killer immune cells scan the body for unhealthy cells, such as cancer. They do this by recognizing and binding specific markers (antigens) on the surface of cells. To be able to differentiate between healthy and cancer cells, killer immune cells use a variety of receptors that bind to specific antigens present in the target cell’s surface. Once the receptors bind their respective antigens they send an activation or inhibitory signal to the inside of the cell. The balance between activating and inhibitory signals tells the killer immune cell if it is in the presence of a cancer or healthy cell, respectively. If the activation signal predominates the killer immune cell will get ready to eliminate the cancer cell. In case the inhibitory signal is stronger the killer cell knows that it is in the presence of a healthy cell and it will move on to the next target. When activating receptors in the killer cell bind cancer antigens they send the activating signal to the inside of the cell through an intracellular activation domain. This activation domain recruits and activates kinases, which in turn will activate other proteins and start a series of signaling cascade events that will lead to the formation of a tight junction between the killer cell and the cancer cell called an immune synapse. Conversely, when an inhibitory receptor binds a normal antigen it will activate its intracellular inhibition domain, which will recruit phosphatases. The phosphatases erase the work of kinases and a killing response will not occur, letting the killer cell move on to check the health of other cells (see Figure 1).
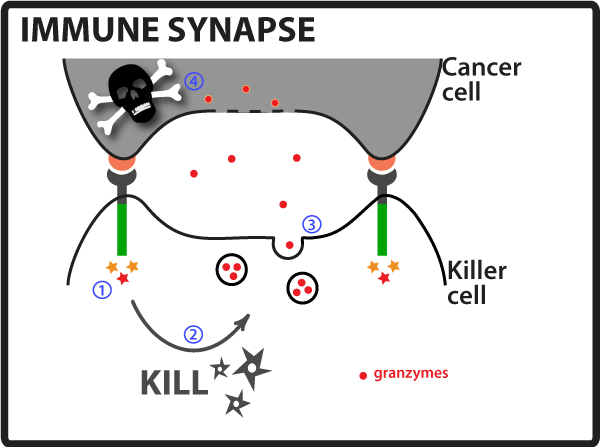
2 - Immune Synapse Formation and Cytotoxic Granules Release Once a killer cell is activated and an immune synapse is formed, the cytotoxic granules present in killer cells get released to act on the cancer cell (see Figure 2). These cytotoxic granules are rich in killing agents, such as granzymes, and once these agents penetrate the cancer cell membrane they will induce the cancer cell to apoptose (kill itself). The immune synapse, a tight embrace between the cancer and killer cell, limits the spread of the killer cell’s arsenal to neighboring, possibly healthy, cells.
Project Aims: Our goals and motivationsTo eliminate cancer more efficiently we thought we could use synthetic biology to engineer synthetic cancer killers that would have improved detection, activation and killing arsenal. For that we would have to modify different steps on the pathway from cancer detection to elimination. Our SYNTHETIC CANCER KILLERS would have:
|
RIGHT CONTENT
replace this area with your content. |
 "
"